Search
- Page Path
- HOME > Search
Original Articles
- Diabetes, obesity and metabolism
- Greater Severity of Steatosis Is Associated with a Higher Risk of Incident Diabetes: A Retrospective Longitudinal Study
- Ji Min Han, Jung Hwan Cho, Hye In Kim, Sunghwan Suh, Yu-Ji Lee, Jung Won Lee, Kwang Min Kim, Ji Cheol Bae
- Endocrinol Metab. 2023;38(4):418-425. Published online July 12, 2023
- DOI: https://doi.org/10.3803/EnM.2023.1729
- 1,220 View
- 77 Download
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
Fatty liver is associated with increased risk of developing type 2 diabetes. We aimed to evaluate whether the severity of hepatic steatosis is associated with incident diabetes.
Methods
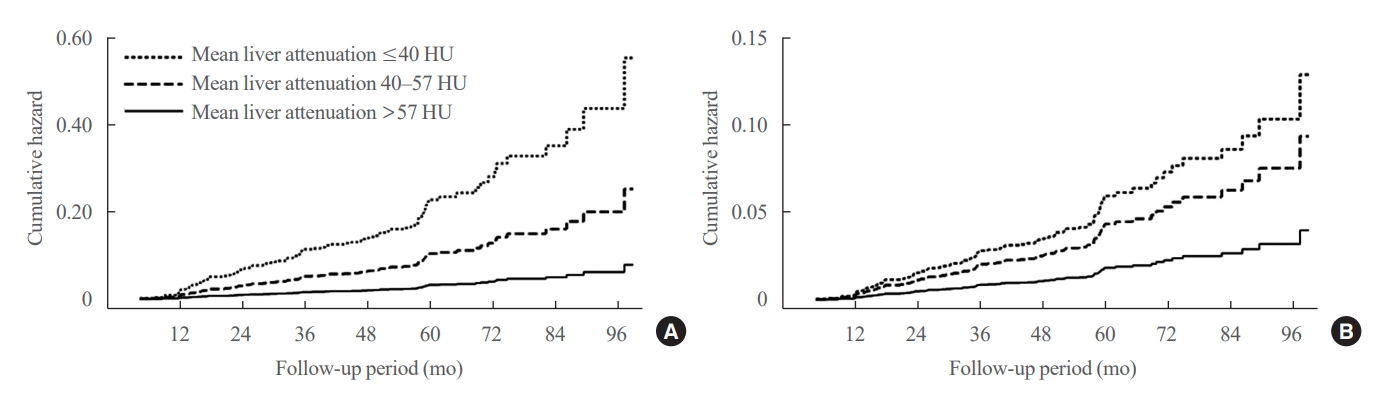
We conducted a longitudinal analysis using data from 1,798 participants who underwent a comprehensive health checkup and abdominal computed tomography (CT). We assessed the association between baseline liver attenuation value on non-contrast CT images and risk of incident diabetes. All the participants were categorized into three groups based on the baseline liver attenuation value on non-contrast CT images: without hepatic steatosis (>57 Hounsfield unit [HU]), mild hepatic steatosis (41–57 HU), and moderate to severe hepatic steatosis (≤40 HU).
Results
During a median follow-up period of 5 years, 6.0% of the study participants progressed to diabetes. The incidence of diabetes was 17.3% in the moderate to severe hepatic steatosis group, 9.0% in the mild steatosis group, and 2.9% in those without hepatic steatosis. In a multivariate adjustment model, as compared with participants without hepatic steatosis, those with moderate to severe steatosis had a hazard ratio (HR) of 3.24 (95% confidence interval [CI], 1.64 to 4.2) for the development of diabetes, and those in the mild steatosis group had a HR of 2.33 (95% CI, 1.42 to 3.80). One standard deviation decrease in mean CT attenuation values of the liver was associated with a 40% increase in the development of diabetes (multivariate adjusted HR, 1.40; 95% CI, 1.2 to 1.63).
Conclusion
We found a positive association between severity of hepatic steatosis and risk of incident diabetes. Greater severity of steatosis was associated with a higher risk of incident diabetes.

- Clinical Characteristics of Langerhans Cell Histiocytosis with Hypothalamo-Pituitary Involvement.
- Eun Shil Hong, Jung Hun Ohn, Jung Hee Kim, Yul Hwang-Bo, Jin Joo Kim, Jung Hee Kwon, Jung Won Lee, Se Youn Choi, Eun Kyung Lee, Sun Wook Cho, Chan Soo Shin, Kyong Soo Park, Hak Chul Jang, Bo Youn Cho, Hong Kyu Lee, Choong Ho Shin, Sei Won Yang, Seong Yeon Kim
- Endocrinol Metab. 2011;26(1):38-43. Published online March 1, 2011
- DOI: https://doi.org/10.3803/EnM.2011.26.1.38
- 1,968 View
- 23 Download
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Langerhans cell histiocytosis (LCH) is a rare disease that involves a clonal proliferation of Langerhans cells. LCH has a predilection for hypothalamo-pituitary axis (HPA) dysfunction, and this leads to diabetes insipidus (DI) and/or anterior pituitary dysfunction. Here, we describe the endocrine dysfunction and clinical characteristics of adult patients with LCH and we analyzed the differences between an adult-onset type and a childhood-onset type. METHODS: The data was obtained from a retrospective chart review of the patients with LCH that involved the HPA and who attended Seoul National University Hospital. The patients were classified into the adult-onset type (age at the time of diagnosis > or = 16) and the childhood-onset type (age at the time of diagnosis < or = 15). RESULTS: Ten patients (9 males and 1 female) were diagnosed with LCH involving the HPA. Five patients were classified as an adultonset type and the other five patients were classified as a childhood-onset type. The median follow-up duration was 6 (3-12) years for the adult-onset type and 16 (15-22) years for the childhood-onset type. All the patients presented with DI as the initial manifestation of HPA involvement. Four adult-onset patients and three childhood-onset patients had a multi-system disease. Panhypopituitarism developed in three adult-onset patients and in one childhood-onset patient. The pituitary lesion of the three adult-onset patients had spread to the brain during the follow-up duration. In contrast, the pituitary lesion of the other two adult-onset patients without panhypopituitarism and all the childhood-onset patients had not changed. CONCLUSION: DI was the initial presentation symptom of HPA involvement. Anterior pituitary hormone deficiency followed in some patients. Compared with the childhood-onset patients, the adult-onset patients were more likely to have panhypopituitarism and a poor prognosis. -
Citations
Citations to this article as recorded by- Pulmonary Langerhans Cell Histiocytosis in an Adult Male Presenting with Central Diabetes Insipidus and Diabetes Mellitus: A Case Report
Yeun Seoung Choi, Jung Soo Lim, Woocheol Kwon, Soon-Hee Jung, Il Hwan Park, Myoung Kyu Lee, Won Yeon Lee, Suk Joong Yong, Seok Jeong Lee, Ye-Ryung Jung, Jiwon Choi, Ji Sun Choi, Joon Taek Jeong, Jin Sae Yoo, Sang-Ha Kim
Tuberculosis and Respiratory Diseases.2015; 78(4): 463. CrossRef - Adult Multisystem Langerhans Cell Histiocytosis Presenting with Central Diabetes Insipidus Successfully Treated with Chemotherapy
Jung-Eun Choi, Hae Ri Lee, Jung Hun Ohn, Min Kyong Moon, Juri Park, Seong Jin Lee, Moon-Gi Choi, Hyung Joon Yoo, Jung Han Kim, Eun-Gyoung Hong
Endocrinology and Metabolism.2014; 29(3): 394. CrossRef
- Pulmonary Langerhans Cell Histiocytosis in an Adult Male Presenting with Central Diabetes Insipidus and Diabetes Mellitus: A Case Report


 KES
KES

 First
First Prev
Prev



